Congenital Central Hypoventilation Syndrome (CCHS)
What is congenital central hypoventilation syndrome (CCHS)?
Congenital central hypoventilation syndrome (CCHS) is a rare and lifelong disorder that affects the central and autonomic nervous system, which controls many of the automatic functions in the body (e.g. heart rate, blood pressure, temperature, bladder and bowel control, etc.). The condition is life-threatening with prompt and adequate treatment.What causes congenital central hypoventilation syndrome (CCHS)?
The underlying cause of CCHS is a mutation in the PHOX2B gene; these mutations are called poly-alanine repeat expansion mutations (PARMs) or non-poly-alanine repeat expansion mutations (NPARMs). Both of these mutations lead to an impaired function of the PHOX2B protein, ultimately resulting in this condition. They are inherited in an autosomal dominant pattern, but can also occur spontaneously.What are the symptoms of congenital central hypoventilation syndrome (CCHS)?
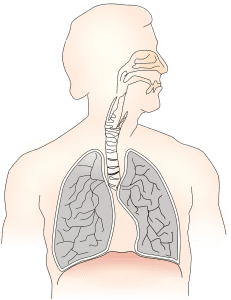
The most recognized symptom of CCHS is the inability of patients to control their own breathing due to a dysregulation of the respiratory drive. This inability varies in severity, but usually, patients experience the most reduced and shallowest breathing during non-REM sleep. Going along with this, individuals with CCHS also cannot sense oxygen or carbon dioxide levels in their bodies, resulting in discoloration of the skin and lips. In addition to the hallmark respiratory problems of CCHS, patients may also have cardiac problems, such as cardiac asystoles (heart stops beating), heart rate variability, altered blood pressure regulation, poor circulation. Digestive problems and ophthalmological problems may also occur.How is congenital central hypoventilation syndrome (CCHS) diagnosed?
After an early recognition of the clinical features of CCHS in an examination and thorough patient and family history, molecular genetic testing can confirm a diagnosis by revealing mutations in the PHOX2B gene.What are the available treatments for congenital central hypoventilation syndrome (CCHS)?
First and foremost, adequate ventilation is essential to ensure the optimal growth and development of CCHS patients and help alleviate the life-threatening respiratory complications with the disease. This ventilation can be managed using a mechanical ventilator via a tracheostomy or mask, or by using phrenic pacemakers. Early detection of CCHS is essential, so patients can start treatment immediately. The cardiac, digestive, and ophthalmological problems associated with CCHS are treated symptomatically and supportively, as they arise.Where can I find more information on congenital central hypoventilation syndrome (CCHS)?
Congenital Central Hypoventilation Syndrome (CCHS) Articles



CCHS Study Highlights Value of Screening Based on Family History
James Moore
April 7, 2020
Read More »

Virginia Tech Super Fan With Rare Disease Uses Twitter to Show Her Love
Jean Martell
November 5, 2019
Read More »
For Patients With CCHS, a Night of Deep Sleep Could Easily be Their Last
James Moore
March 4, 2019
Read More »

Active Man Sets an Example of The Success of Mechanical Ventilation Technology
James Moore
March 27, 2018
Read More »

Parenting a Child with Rare Disease: The Trials and Tribulations
Andres Rovira
September 29, 2017
Read More »


