According to Bronchiectasis News, patients with both HIV and bronchiectasis often have a difficult time being diagnosed with the respiratory condition. After researchers examined data from 14 patients, they discovered that patients are misdiagnosed and not referred to the specialists who can give them the targeted medications and therapies needed. Read the full study in Case Reports in Pulmonology.
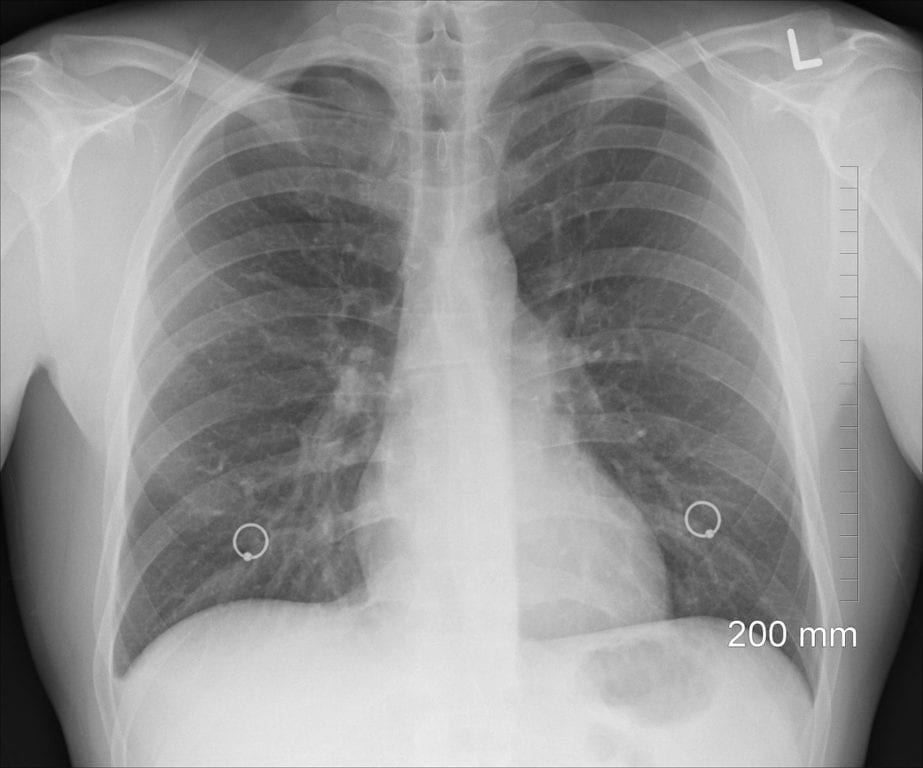
Bronchiectasis
Bronchiectasis is a pulmonary condition in which the lung’s bronchial tubes are damaged, thickened, or widened. When this occurs, bacteria and mucus can build up in the lungs, making it more difficult to breathe.
Bronchiectasis can be cystic fibrosis or non-cystic fibrosis. Non-CF causes include HIV, autoimmune disorders, alpha-1 antitrypsin deficiency, rheumatoid arthritis, and inflammatory bowel disease (IBD).
Symptoms of bronchiectasis include a daily cough, weight loss, chest pain, and coughing up blood or mucus. Learn more about bronchiectasis.
Patients with HIV
HIV
Human immunodeficiency virus (HIV) is a virus that attacks cells in the body that help fight infection. It kills off CD4-positive T-cells, a type of lymphocytes (immune cells). People without HIV have a CD4 count between 500 and 1600 cells per cubic millileter. This may drop in someone with HIV. However, if the disease progresses to acquired immunodeficiency syndrome (AIDS), CD4 count drops under 200. Learn more about HIV.
The Study
To understand how HIV and bronchiectasis intersect, researchers explored 14 medical records sourced over a 19-year period. Patient demographics included:
- Patients between the ages of 12 and 77.
- 12 patients (86%) were women.
- 5 patients had a CD4 count over 500.
- 4 patients had a CD4 count between 200-500.
- 5 patients had AIDS.
Patients were not initially treated for bronchiectasis. Instead, initial diagnoses included:
- A fungal lung infection – 1 patient
- Asthma – 1 patient
- Chronic obstructive pulmonary disease – 3 patients
- Fungal pneumonia – 6 patients
- Mycobacterium avium complex, a bacterial infection – 7 patients
Treatments included antimicrobials, which could harm patients by getting rid of healthy bacteria. However, many patient lung scans were not passed onto specialists or primary care physicians.
Future Treatment for Patients with HIV and Bronchiectasis
The first step in adequately treating these patients is early identification and specialist referrals. Next, doctors must plan on ways to assist marginalized populations. Many of the patient data gathered for this study was from patients in geographical areas with higher levels of poverty and less access to care.
In this case, researchers determined that:
“bronchiectasis can carry a significant symptomatic burden”
for patients with HIV. However, even a study of the research shows that in 20 years, only 14 patients with HIV also received a bronchiectasis diagnosis. As such, it is likely that many more patients have undiagnosed bronchiectasis, or are not being given proper treatment. So pulmonologists working with these patients must consider bronchiectasis as a possible diagnosis in the face of respiratory symptoms.
What are your thoughts on these findings? Share your stories, thoughts, and hopes with the Patient Worthy community!