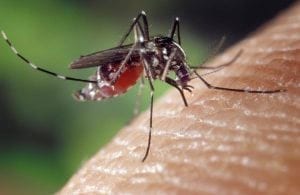
The Plasmodium vivax (P. vivax) parasite commonly leads to malaria infection. In fact, around 7.5 million malaria cases result from the parasite. But the tricky part about P. vivax is that it can stay dormant in the body for years. When it suddenly reappears, patients experience a reemergence of symptoms and lowered quality of life. However, researchers recently learned more about the P. vivax life cycle, leading to more effective treatment in the future. Check out the full findings of their study published in Malaria Journal.
Malaria
Malaria is a mosquito-borne illness caused by parasitic infection. Generally, the parasite infects humans following a mosquito bite. However, blood infusions, sharing needles, and traveling to high-risk countries also raise the risk. While cases are more common in areas such as South Asia or sub-Saharan Africa, only 1,700 Americans get malaria each year.
Symptoms include:
- A persistent cough
- Chest and abdominal pain
- Sweating and chills
- Nausea
- Vomiting
- Severe headaches
- High fevers
- Flu-like symptoms
- Fatigue
- Muscle aches
If left untreated, malaria can lead to anemia, organ failure, or death. Learn more about malaria here.
Proof-of-Concept Study
India is home to over half of all malaria cases. But despite the parasitic infection being so widespread, you might be surprised to read that there is only one drug designed to combat P. vivax’s impact on the liver. However, this drug is not well-tolerated and not safe for use in pregnant women or children.
Researchers wanted to understand how P. vivax impacted the liver. First, they cultured human liver cells in their lab. Next, researchers bred mosquitoes, feeding them with infected blood. Finally, after removing parasites from the mosquitoes, researchers infected liver cells with P. vivax.
In doing so, researchers discovered that:
- Cells taken from patients with liver cancer, or patients who needed biopsies, did not experience large-scale infections.
- Liver cells created from pluripotent stem cells were not more susceptible to malaria.
- Testing cells gave insight into whether a patient would respond to certain treatments.
- UIS4, a malarial protein, utilized LC3, a human protein, for protection.


-300x300.jpg)