Twins have always been a thing that has mystified the world, intrigued people, and definitely a curiosity. Fraternal, Identical, and everything in between – multiple births are a source of fascination. But why should we raise awareness of the complications, and in particular, of twin anemia polycythemia sequence (TAPS)?
Shared Placentas Cause Different Problems
Within the twin world, there are many different complications. The most well-known is twin to twin transfusion syndrome, found in twins sharing a placenta. Blood is transferred from one twin to the other via large surface connections in the placenta, causing fluid imbalances.
Selective fetal growth restriction is a lesser-known related disease. It’s also called selective intrauterine growth restriction. This is where the placenta is shared unequally or where cord insertions impede the growth of one baby. This is characterized by one baby being smaller than the other.
Both these diseases should be taken seriously and screened for regularly. Most guidelines around the world support routine screening for monochorionic twins (those sharing a placenta) every 2 weeks, with fluid checks, umbilical dopplers to check the health of the placenta, along with the usual routine examinations.
But there is a third, much more controversial diagnosis.
Twin Anemia Polycythemia Sequence
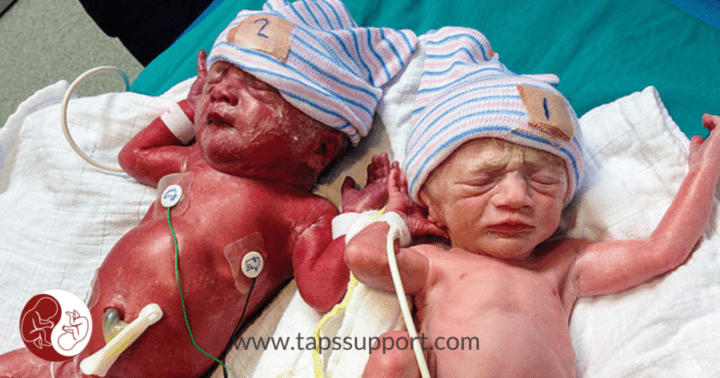
In March 2006, 2 papers were released within days of each other. The first described a complication of successful TTTS laser surgery, where one twin would be born anemic and the other polycythemic. Small, residual connections in the placenta that were either missed or incompletely sealed in the process were the cause of this problem.
The second paper described the same condition but as happening spontaneously. This cornerstone article also gave the disease a name – twin anemia oolycythemia sequence, or TAPS.
TAPS is a rare disease, affecting just 3-5% of monochorionic twins in its spontaneous form and happening in between 0-16% of post-laser TTTS cases. It is detected through dopplers done on the mid-cerebral artery (MCA) of the babies and via other ultrasound indicators. It can also be diagnosed after birth using blood counts (hemoglobin and reticulocytes) and placenta pathology.
Treatments
Right now, the best treatment for TAPS is unknown. Several treatment options are available, including laser surgery, in-utero transfusions, expectant management (or watch and wait), early delivery, or selective reduction.
An international, multicentre trial has been established to help determine the best treatment for TAPS, placing laser surgery against conventional treatment options.
After birth, TAPS is generally treated through blood transfusions and partial exchange transfusions.
Short and Long Term Outcomes
We need to break it down into post-laser TAPS and spontaneous TAPS here. Both have serious consequences but very different short and long-term outcomes.
In post-laser TAPS, long-term outcomes are similar to TTTS, with severe neurodevelopmental impairment at around 9%. But in relation to perinatal mortality, 26% of TAPS donors are at risk of dying in utero or just after birth.
In spontaneous TAPS, donors are also at risk of death (12%), but the long-term effects are devastating. 35% of TAPS donors will have some degree of cognitive impairment, and 15% of donors will be born deaf due to auditory neuropathy spectrum disorder.
TAPS is by no means a mild disease as was once thought. However, routine screening for TAPS is still not part of screening protocols, and many myths persist.
Breaking Down Myths
One of the biggest myths about TAPS is that it’s a form of TTTS. This is not true. Both have different staging systems, different diagnostic criteria, and different long-term outcomes. It can also create confusion – patients who have twins sharing a placenta may ask if they’re being screened for TTTS and assume this covers TAPS as well. We need to acknowledge that ever since the beginning, TAPS and TTTS have been recorded as being separate, distinct diseases.
Many guidelines worldwide still do not support routine TAPS screening. Citing either a lack of established treatment protocols or not enough evidence, this means that many families are faced with the prospect of undiagnosed TAPS.
Despite 15 years of research into this disease and with more and more information about TAPS coming to light, these tired guidelines still deny families routine screening.
Why Is It Important To Know About TAPS?
It may be a rare disease, but TAPS families often feel lonely in their diagnosis. We struggle with uncertainty about our kids’ futures, with many families affected by cognitive delays and other issues from TAPS and the prematurity associated with our disease.
We’re often called paranoid or our concerns about our children are dismissed because there’s a lack of knowledge about our disease. Stay off Google! Don’t listen to the mom groups – because now that they’re born, everything is ok!
As parents of TAPS twins, we know a little about our disease, but the long-term effects are devastating. We also live with the knowledge that the subsequent significant finding could be around the corner and that we don’t know what this will bring us.
We’re the little kid at the concert, standing behind the TTTS crowd trying to be recognized for our own disease.
Compassionate online communities exist, like this one to help families advocate, but the urgency lies with updating screening protocols worldwide. The TAPS Support Foundation does this through their Facebook group and providing free resources on their website.
TAPS is a very real disease with serious long-term consequences. It’s not a form of TTTS but its own distinct entity. We need to raise awareness for TAPS and start advocating for routine screening for it for monochorionic twins.
After all, TAPS is Real.