According to a story from cbc.ca, Michelle Boich, 33, was facing the prospect of blindness if she is unable to get access to a crucial procedure that could treat her case of keratoconus. Ironically, Michelle works as an optometric assistant, helping maintain the eye health of others– and yet she couldn’t find treatment for her own vision problem.
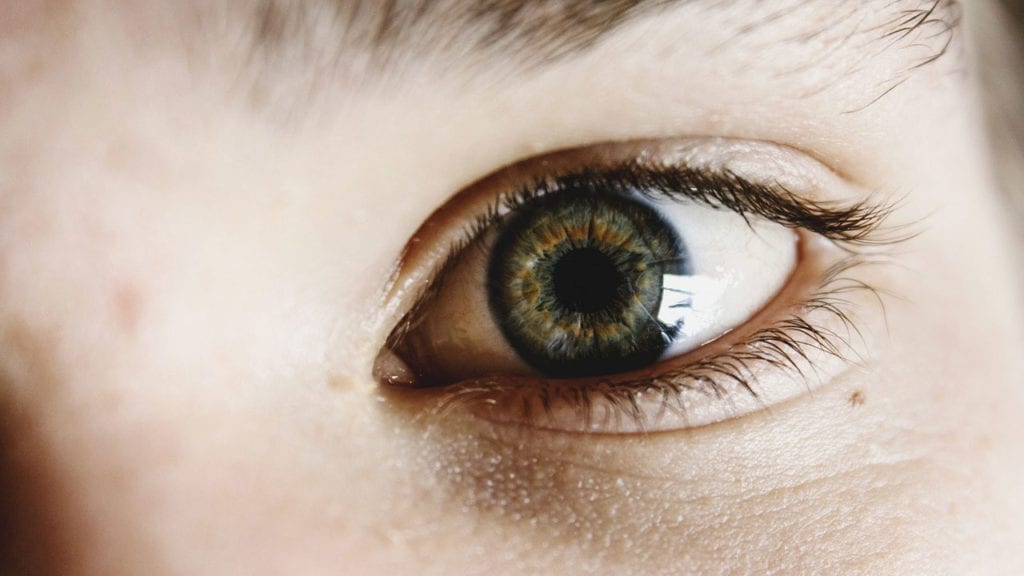
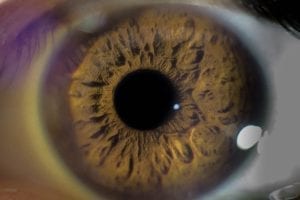
Keratoconus is an eye disorder which results in the thinning of the cornea over time. Typically both eyes are affected. The disorder is often diagnosed in early adulthood. Common symptoms of keratoconus include double vision, blurred vision, light sensitivity, nearsightedness, and astigmatism. A diagnostic complaint can be the appearance of multiple “ghost” images surrounding a given object. The cause of keratoconus is not well understood; a variety of environmental, hormonal, and genetic factors could play a role. In the beginning stages, keratoconus can be corrected similarly to standard vision loss with eyeglasses or contacts. However, as the disease progresses, more specialized contacts may be needed. In severe cases, corneal transplants or other surgery may be necessary to prevent vision loss, as corrective methods will not slow progression of the disease. To learn more about keratoconus, click here.
Michelle did not want to have to wait for her vision to decline to the point that she will have to seek transplant surgery. The truth of the matter is that she should not have to; a more recent procedure, called corneal collagen cross linking (CXL) serves to strengthen the cornea. This could halt the progression of her disorder and could even reverse some vision loss.
Initially, it seemed like she was not going to be able to get the CXL procedure; after conducting a pilot program, Ontario has spent $800,000 to cover CXL for qualifying patients, but the requirements to be eligible were not easy. Michelle had amblyopia (lazy eye) when she was kid, and this was enough to disqualify her at first.
However, fortunes have recently shifted in her favor. She was able to qualify for the Kensington Program which put the operation within her price range. Now, Michelle is scheduled to get CXL for both of her eyes as well as phototherapeutic keratectomy (PTK) for her weaker left eye. For six months after the surgery, Michelle will wear glasses to help stabilized and correct her vision; through this healing period, her eyesight will change rapidly.
Meanwhile, Ontario province is in the process of getting a diagnostic code that will ensure that CXL will be available and affordable to everyone and not just limited to few locations.