As stated in a press release from the University of Illinois at Urbana-Champaign, researchers have discovered a bacterial protein fragment that is destructive to lung tissue. This can rapidly worsen complications of idiopathic pulmonary fibrosis.
By recognizing that there is a bacterial component to idiopathic pulmonary fibrosis, researchers are hopeful that they can create more targeted therapies for patients. You can find the full study published in Nature Communications.
What is Pulmonary Fibrosis?
Pulmonary fibrosis is a condition in which the lungs become scarred. Symptoms include shortness of breath, weight loss, muscle aches, and fatigue. As the condition progresses, additional complications can include heart failure, lung infections, and blood clots.
While pulmonary fibrosis can broadly be caused by chemical exposure or medications, idiopathic pulmonary fibrosis (IPF) refers to the condition when it occurs with an unknown cause. The lung tissue hardens and scars, making it difficult for the blood to get enough oxygen. IPF affects up to 20 out of every 100,000 people worldwide.
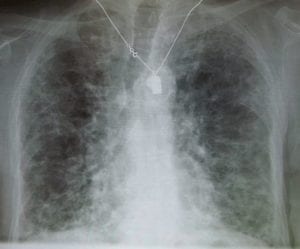
However, IPF can sometimes develop slowly, making it difficult to receive an early diagnosis. As a result, life expectancy after diagnosis averages around 3-5 years. Previously, researchers hypothesized that IPF could be caused by viral infections or genetic mutations. Learn more about idiopathic pulmonary fibrosis here.
The Study
As stated earlier, IPF conditions can be on the milder side until the condition progresses. Then patients may experience “acute exacerbation,” a period of rapid symptom worsening. During this time, patients will lose lung function and have a more difficult time breathing.
Researchers wanted to understand why patients in previously stable conditions could suddenly experience acute exacerbation. This is especially important because this event is fatal in the moment for 50% of patients, with 50% fatalities experienced in the next 4 months.
Bacteria
Previous research suggested that certain types of bacteria rapidly increased within the lungs of patients with idiopathic pulmonary fibrosis. Researchers believed that these bacteria – strains of Halomonas, Staphylococcus, and Streptococcus – were dependent on high levels of salt in lung tissue and lung lining.
To test their theory that these bacteria may trigger acute exacerbation, researchers created cultures with strains of the bacteria seen in lung tissue of patients with IPF. They examined these cultures within a high-salt environment.
Microbiology professor Isaac Cann stated:
“We discovered salt-loving bacteria in the lungs of patients with pulmonary fibrosis, and these bacteria secrete a peptide that marks the lung cells it touches for death.”
Corisin
Through the cultures, researchers found that the strain Staphylococcus nepalensis was secreting a peptide, which they named corisin. It was determined that corisin destroyed lung cells, making it much more likely for patients to experience acute exacerbation.
Lung tissue samples taken from patients showed a higher level of corisin after acute exacerbation. Additionally, a study run on mice with idiopathic pulmonary fibrosis found that mice injected with Staphylococcus nepalensis or corisin were more likely to show signs of acute exacerbation over control mice or mice injected with another strain of Staphylococcus.
Genomes
Researchers sequenced the Staphylococcus nepalensis genome to better understand where corisin develops in the body. Corisin is initially a part of a larger protein. However, once separated, this bacterial fragment begins killing tissue. Upon testing, it was discovered that the larger protein did not share the same destructive properties.
Currently, it is unclear what enzyme is responsible for separating corisin from its larger protein.
Next Steps
Researchers aim to conduct additional testing to narrow down what enzyme cuts corisin off of the larger protein. In doing so, researchers can create more targeted therapies, drugs, and treatments for those with idiopathic pulmonary fibrosis.
Immunology professor Esteban Gabazza has hope for the future, stating:
“On the patient side, this new discovery could mitigate the psychological stress of fighting against an ‘unknown intruder,’ while on the physician side, this can stimulate the development of strategies for treatment.”
This type of research is crucial to not only IPF, but also other diseases and disorders who might be shaped or worsened by bacterial sources. Finding the enzyme will help researchers craft a medication to block it, preventing the enzyme from separating corisin and its protein, and thus better protecting lung tissue.
Researchers also hope to discover whether other bacteria can create corisin, or if corisin and bacteria have causal links to fibrosis in other areas of the body. Additionally, there is a possibility that COVID-19 infection and recovery can lead to pulmonary fibrosis. Better understanding the condition will better poise researchers to address a potential increase in diagnoses.






