Cancer screenings are very important for early detection, which can then lead to treatment administered earlier in disease progression and better outcomes. Pancreatic cancer is no exception. In fact, this cancer is often difficult to detect early, and patients do not receive a diagnosis until it has already progressed. To combat this problem, Mission: Cure has released some guidelines on pancreatic cancer screening so that you can be best educated.
About Pancreatic Cancer
Pancreatic cancer occurs in the pancreas, an organ that is responsible for a number of enzymes and hormones. These aid in various processes throughout the body, such as digestion and maintaining blood sugar. There are multiple forms of pancreatic cancer, depending on which part of the organ is impacted. The two main types are exocrine pancreatic cancer and pancreatic neuroendocrine tumors. Regardless of type, symptoms include unintentional weight loss, diabetes, blood clots, dark urine, pain in the upper abdomen and back, jaundice, a loss of appetite, fatigue, bowel obstruction, and depression.
Doctors are unsure as to what causes this cancer; they only know that cells begin to grow and multiply out of control until they form a tumor. This lack of knowledge can make it difficult to diagnose and treat pancreatic cancer, which is already notoriously hard to diagnose. Affected individuals often do not notice symptoms until the cancer has already progressed, meaning that a diagnosis does not come until the cancer is in its later stages. Once diagnosed, treatment options include surgery, targeted therapy, radiation, chemotherapy, and supportive care.
What is Pancreatic Cancer Screening?
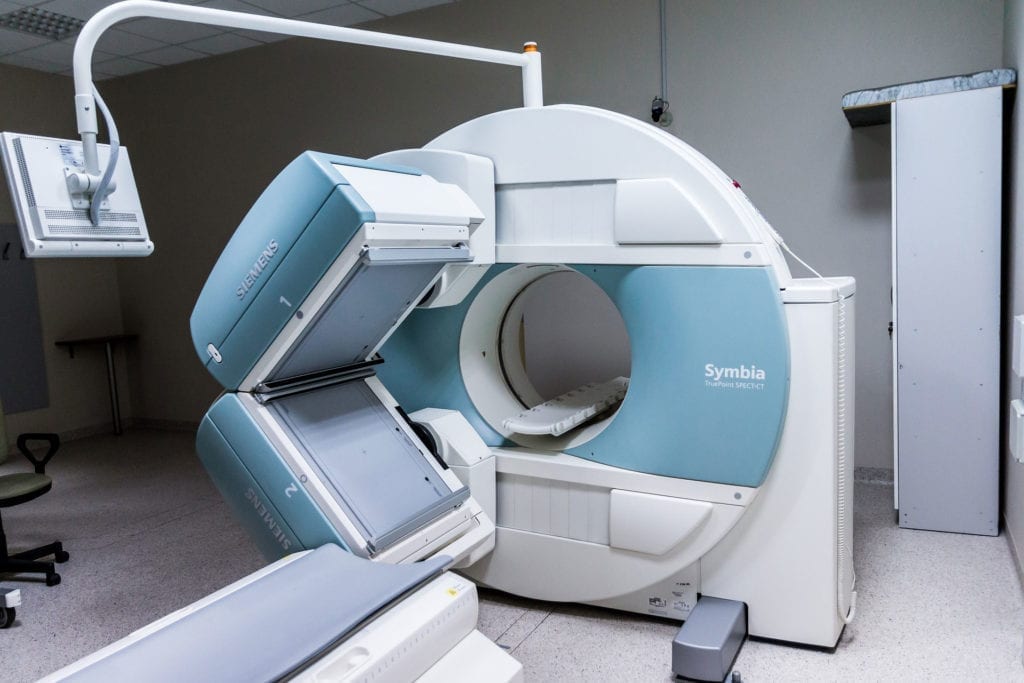
Screening for this cancer consists of MRIs and endoscopic ultrasounds (EUS). CT scans may also be used. It is often challenging to thoroughly screen, as tumors in the pancreas can be difficult to see, especially in the early stages. That is why regular screening (every 12 months) is so important.
Who is at Risk of Pancreatic Cancer?
Research has shown that people affected by chronic pancreatitis are at an increased risk of developing pancreatic cancer, with a 5% chance over 20 years. Dr. Randall Brand, the head of the early pancreatic cancer detection program at the University of Pittsburgh Medical Center, notes that this risk is not evenly distributed throughout chronic pancreatitis patients. Those with PRSS1 and some CFTR mutations stand at a higher risk, although more research needs to be done into this topic.
Because of the heightened risk that people with these mutations face, physicians recommend that they are screened for this cancer regularly, starting at age 40. Similarly, people with genetic variants related to pancreatic cancer should be screened regularly starting at age 50. These variants include the BRCA1 and BRCA2 genes. Lastly, people with two or more relatives affected by this cancer should begin screening at age 50 or ten years before their relatives were diagnosed.
What Can I Do to Prevent Pancreatic Cancer?
While regular screenings can lead to better outcomes, there are things that can be done to prevent pancreatic cancer as well. Medical professionals advise avoiding smoking, following an exercise routine, eating a healthy diet that includes fruits and vegetables, and losing weight if necessary. Even if you incorporate these tips into your life, make sure that you are still screened once a year if you live with an increased risk of pancreatic cancer!