As many patients in the rare disease community know, achieving a diagnosis can be a lengthy and difficult journey. Following this journey, it can still take a while to receive appropriate treatment. According to the National Hemophilia Foundation (NHF), new clinical guidelines are now available designed to combat these difficulties for patients with von Willebrand disease (VWD). The guidelines were developed by the NHF in conjunction with the World Federation of Hemophilia, the International Society on Thrombosis and Haemostasis, and the American Society of Hematology. See the full set of guidelines published in Blood Advances.
Von Willebrand Disease (VWD)
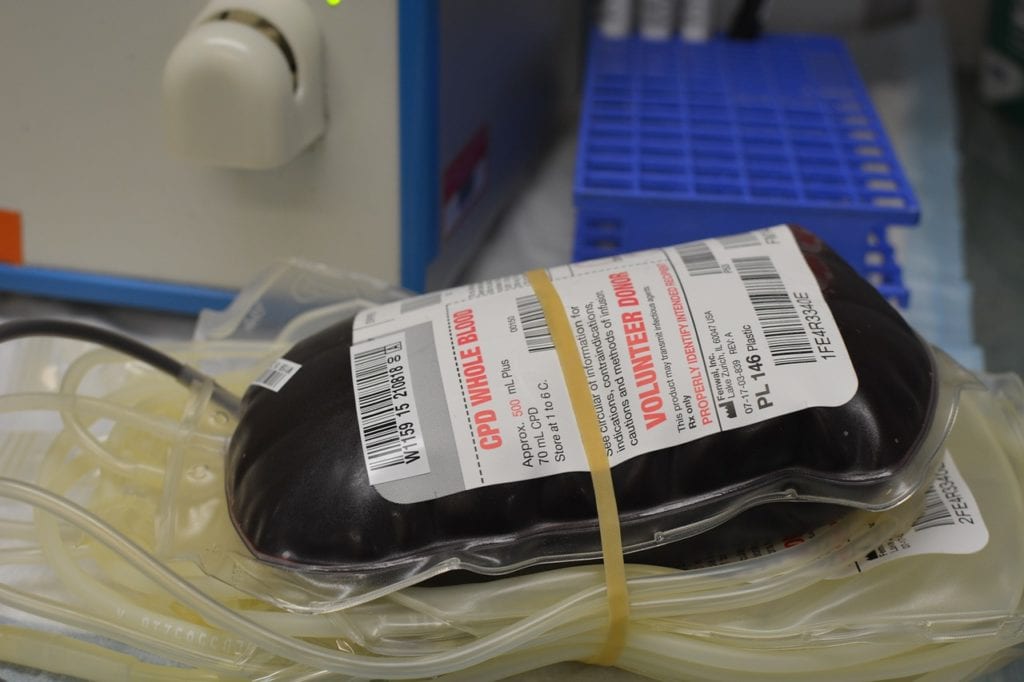
von Willebrand disease (VWD) is a rare, but the most common, bleeding disorder that impacts the blood’s clotting ability. It is named after Erik von Willebrand, who first discovered and defined VWD in 1925. Over 300 VWF gene mutations cause VWD. With this conditions, patients’ blood is von Willebrand factor (VWF) deficient. Normally, VWF carries factor VIII, a blood clotting factor, into the blood. VWF also helps clot platelets together to seal blood vessel holes. Without enough VWF, patients often bleed easily and excessively.
An estimated 1 in every 100 to 10,000 people has VWD. The condition affects both males and females. However, females are more likely to recognize symptoms, particularly around menstruation or childbirth.
VWD Types & Symptoms
There are three forms of VWD. First, Type 1 VWD, which makes up about 75% of diagnoses, is characterized by low VWF levels. Typically, this form is relatively mild.
Next, Type 2 VWD is moderately severe. While these patients have enough VWF, it does not work properly. Patients with Type 2A have a protein defect that prevents blood platelets from binding together. In Type 2B, VWF binds to platelets within the bloodstream rather than at the injury site. With this subtype, thrombocytopenia (or a low platelet count) is common. In Type 2N, a rare subtype, VWF works normally with platelets, which clot at the injury site. However, this fails to put FVIII into blood circulation, causing VWF deficiency.
Finally, Type 3 VWD is the most rare and severe form. In this form, patients have little or no VWF.
In many cases, patients with VWD only experience mild symptoms. However, if symptoms do appear, they include:
- Easy bruising, which could signify internal bleeding
- Joint or muscle pain, stiffness, and inflammation
- Limited movement
- Bloody urine or stool
- Frequent and difficult-to-stop nosebleeds
- Bleeding from the gums
- Excessive bleeding following dental procedures, shaving, or other mild injuries
- Excessive, heavy, and long-lasting menstrual flow
Clinical Guidelines
Unfortunately, VWD can be difficult to diagnose and care for. This is especially true because VWD ranges in symptoms, severity, and presentation. Because of this, the above organizations determined that new clinical guidelines were needed to ensure patients received the highest quality of care. Altogether, 32 individuals on two expert panels assisted in creating these guidelines. These panels included patients with VWD, hematologists, and scientists. After developing clinical questions, these were introduced to an international panel. Following a survey, the ideal questions were identified.
Next, the University of Kansas Medical Center reviewed evidence, which was later used by the panel to create recommendations for the clinical guidelines. Because there was not a lot of evidence, the panel also believes more research into VWD is needed. Altogether, 19 recommendations make up the clinical guidelines. These include:
- For patients with a high probability of VWD (eg, affected first-degree relative), the panel recommends against relying on a BAT to decide whether to order specific blood testing (strong recommendation based on moderate certainty in the evidence from diagnostic accuracy studies).
- In patients with VWD with a history of severe and frequent bleeds, the guideline panel suggests using long-term prophylaxis rather than no prophylaxis (conditional recommendation based on low certainty in the evidence of effects).
Once the guideline becomes more readily available, the publishing organizations will also offer additional resources to streamline implementation.