Hypereosinophilic syndrome (HES) patients may finally have a meaningful treatment option. According to an article published at BusinessWire.com, AstraZeneca’s FASENRA (benralizumab) has shown statistically significant efficacy in delaying disease progression, offering hope to individuals suffering from this rare and potentially life-threatening condition characterized by dangerously elevated white blood cells called eosinophils.
Understanding the Disease Challenge
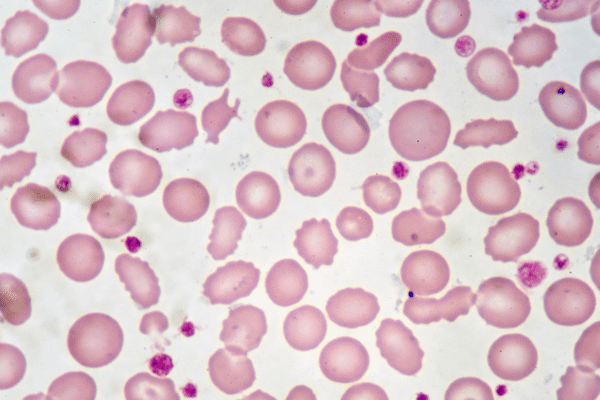
HES is a group of rare disorders characterized by persistently elevated eosinophil levels in the blood, leading to organ and tissue damage that can prove fatal if untreated. The disease presents with a bewildering array of symptoms—including fatigue, fevers, night sweats, chest pain, and neurological complications—making diagnosis difficult and patient management exceptionally challenging. Current treatment options are limited, relying on glucocorticosteroids, chemotherapy, tyrosine kinase inhibitors, and other immunosuppressive agents that carry significant side effects and often provide inadequate symptom control.
NATRON Trial: Landmark Results
The Phase III NATRON trial, involving 133 patients randomized to receive either monthly 30 mg subcutaneous injections of FASENRA or placebo, met its primary endpoint convincingly. FASENRA reduced the risk of disease worsening or flares by 65%, with only 19.4% of patients experiencing flares compared to 42.4% in the placebo group. This statistically significant result represents a meaningful breakthrough for patients desperately seeking effective disease management.
Comprehensive Secondary Benefits
Beyond the primary endpoint, FASENRA demonstrated impressive results across multiple secondary measures. Only 22.4% of treated patients experienced flares or withdrew from the study compared to 45.5% in the placebo group. The annualized flare rate dropped dramatically to 0.41 flares per year with FASENRA versus 1.23 per year with placebo—a 66% reduction. Perhaps most notably, FASENRA delayed hematologic relapse with a hazard ratio of just 0.08, indicating substantial clinical benefit.
Symptom Relief and Quality of Life
One particularly important finding concerns fatigue, a debilitating symptom affecting many HES patients’ quality of life. Beginning by Week 4 and continuing through Week 24, patients receiving FASENRA showed significantly greater improvements in fatigue scores compared to placebo. This sustained symptom relief may enable patients to resume normal daily activities and improve their overall well-being—benefits that extend far beyond preventing disease flares.
Safety and Clinical Implications
The safety and tolerability profile remained consistent with FASENRA’s established safety record in other eosinophilic conditions, meaning physicians can prescribe this treatment with confidence. The convenience of monthly injections also distinguishes FASENRA from more burdensome existing therapies.
Future Impact
These results represent a transformative moment for HES patients with very limited current options. FASENRA’s proven ability to address eosinophilic inflammation positions it as a potential new standard of care. With regulatory filings in progress and presentations planned for major medical conferences, including the American Society of Hematology’s December 2025 meeting, widespread availability appears imminent.
For patients enduring HES’s unpredictable symptoms and organ damage risks, FASENRA offers genuine hope, backed by rigorous clinical evidence, that disease progression can be effectively managed with a simple monthly treatment regimen.