Annie and Peter McKenzie describe their seven-year-old son Patterson as having a “heart of gold.” Patterson is bright, funny, happy, and empathetic. Despite his insistence that he is not a sports lover, Patterson enjoys baseball and golf. He spoke animatedly about his love of legos, being lazy around the house, their new dog Bruce, and math, which is his favorite subject at school (even though he also loves reading and writing). Patterson plays the piano, does karate, and likes to practice swimming. When it comes to living life to the fullest, it’s clear that Patterson doesn’t let his recessive dystrophic epidermolysis bullosa (RDEB) diagnosis get him down.

Of course, living with RDEB can be difficult – and sometimes isolating. There are a number of challenges associated with RDEB. It can take hours each day to bandage wounds. Patterson sometimes has to miss out on birthday parties or events. And there are currently no FDA-approved treatment options for those with epidermolysis bullosa. But the McKenzie family is not giving up on finding a cure in Patterson’s lifetime. From launching Pursuit for Patterson to sharing Patterson’s story on Patient Worthy, the McKenzies are doing all that they can to raise EB awareness – and show others that they are not alone.
In our interview, Annie, Peter, and Patterson talk about what RDEB is, Patterson’s story, finding advocacy connections, the importance of research, and advice for families facing new diagnoses.
What is Epidermolysis Bullosa (EB)?
Epidermolysis bullosa (EB) refers to a group of connective tissue diseases which cause moderate-to-severe skin blistering. Dystrophic epidermolysis bullosa (DEB) falls under that greater umbrella; DEB can be further broken down into dominant (DDEB), recessive severe generalized (RDEB-sev gen), or generalized and localized recessive (RDEB-gen and -loc). RDEB-sev gen is considered the classic and most severe form. In Patterson’s case, his RDEB is considered intermediate. Annie explains:
RDEB is a connective tissue disorder that ultimately impacts his skin, but also affects the digestive tract, mouth, esophagus, cornea, nail beds, all the way down to the organs. It can be complex depending on the level of severity and, in some cases, life-limiting and life-threatening. The skin is very fragile and even minor friction, like wearing clothes, can cause Patterson’s skin to blister or shear off. Some trauma situations, like falling at recess, can pretty severely impact his skin and body.
RDEB results from COL7A1 gene mutations. Normally, this gene encodes for the production of subunits of type VII collagen. This collagen plays a role in connective tissue structure and strength. RDEB is inherited in an autosomal recessive pattern, meaning someone affected must inherit one mutated gene from each parent. As Annie explains:
Peter and I are both carriers, which was really shocking to us. We had never heard of RDEB before Patterson’s diagnosis.
RDEB Symptoms
Symptoms related to RDEB can (but do not always) include:
- Malformed or missing fingernails and toenails
- Difficulty swallowing (or other feeding difficulties)
- Slow growth
- Eye inflammation
- Fused skin between the fingers and toes
- Hair loss
- Thin-appearing skin
- Joint contractures
- Painful or itchy skin
- Blistering and scarring on the hands, knees, elbows, feet, other areas of the body, and mucous membranes
- Increased risk of squamous cell carcinoma
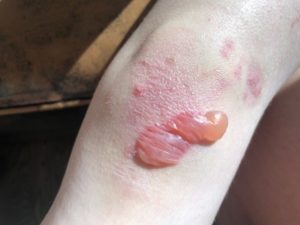
Patterson explains:
My body gets scraped. We take good care of it but it does sting a little bit in baths sometimes.
Patterson’s Story
When Patterson was first born, he already showed signs of epidermolysis bullosa. He was missing skin on his fingers, causing doctors to wonder if Patterson had been sucking on his thumb in the womb. Later, while sitting in the bassinet, Patterson hit his heel. A blister formed, piquing the doctors’ interest. Annie explains:
The doctors couldn’t diagnose it themselves. We spent a week in the hospital. They were really hesitant to release us and even wore hazmat suits for our final day. But since Patterson was otherwise thriving, they seemed to not be overly concerned. Before we left, we were referred to a pediatric dermatologist to find a diagnosis.
One week later, the family met with a pediatric dermatologist who immediately suspected that Patterson had epidermolysis bullosa. According to Peter:
She tried to shear his skin a little or create a blister. It really made Patterson mad. But she couldn’t create a blister immediately. So that made the potential EB diagnosis kind of questionable. We waited until a later date when he had blistered skin and had that biopsied. The sample was sent to Stanford and that came back with RDEB. We also found out that he has a slight amount of collagen in the epidermis level of his skin, so he has some binding. That’s why, now, we see blisters on more ‘high traffic’ areas and from falls, scrapes, and slips. But that depends. Sometimes he’ll fall and get up with no blistering, and others he’ll have huge blisters just from sleeping in bed. It’s hard to predict.
After receiving the official diagnosis, the dermatologist told Annie and Peter that they would become the experts on RDEB and would most likely have to teach doctors about the disease. Annie shares:
That was isolating. You expect medical professionals to tell you what to do along the way. But we had to figure out bandages, techniques, what blisters to pop and what to keep.
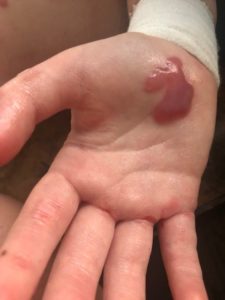
However, the doctor did point the McKenzie family in the right direction. Annie and Peter were told not to Google the condition. Rather, the doctor told them to check out the Dystrophic Epidermolysis Bullosa Research Association of America (DEBRA), an organization which supports the EB community. Through DEBRA, Annie and Peter were able to register and receive a kit with bandaging supplies and information.
Taking Care of RDEB
So what is the process of caring for RDEB-associated blistering? First, the family keeps Patterson’s skin moisturized to try to reduce itching and improve healing. Annie explains that they also use a variety of other tools and products:
We have razors to pop the blisters. We want to pop them as soon as we see them form because he doesn’t have enough collagen to stop the spread, so the blisters will just continue to grow without intervention. After that, we put Bacitracin on the wound if it’s ‘angry’ or bleeds. Then we put Aquaphor or petroleum jelly on non-adhering mesh, place that directly on the wound to keep it moist, and then wrap it with gauze. We put the Mepilex liner on top to hold everything together. We can also use Mepilex on the heels or toes as a protective layer.
While attending one of the DEBRA conferences, Annie and Peter learned that some other children and families place Mepilex directly on open wounds. However, this has not been successful for Patterson; because it has some adhesive properties, the Mepilex can somewhat stick to the wound and cause pain or discomfort. Annie says:
It’s crazy because even with the exact same diagnosis and subtype, what works for us isn’t always what works for other people. So you have to find your routine and stick with it. This is really the only treatment that we have for our children right now. Bandaging prevents reinjury and infection. But it can also be incredibly expensive. Our insurance hasn’t covered it so we have to pay out of pocket. The average family pays $10,000 monthly for bandaging.
Patterson’s jaw dropped when his parents mentioned that they spend around two hours each day bandaging his wounds. They have a morning routine to get him prepared for school (after all, the life of a first grader can be very busy and active!), as well as a nightly routine to assess any potential injuries or blistering developed during the day.
In terms of pain management, the family uses Tylenol. Peter explains:
We tend to use distraction methods for the day-to-day pain management from bandage changes: things like singing, reading, watching a favorite show on the Ipad. In kids with more severe cases, there are additional pain management options.
Baths can also be very painful, especially when wounds are healing. Sometimes, Patterson takes bleach baths or isotonic baths, which can help with healing and pain reduction.
Join us in Part 2 as Annie, Peter, and Patterson share how they advocate and take action for recessive dystrophic epidermolysis bullosa awareness, as well as their advice for other families on this journey.






