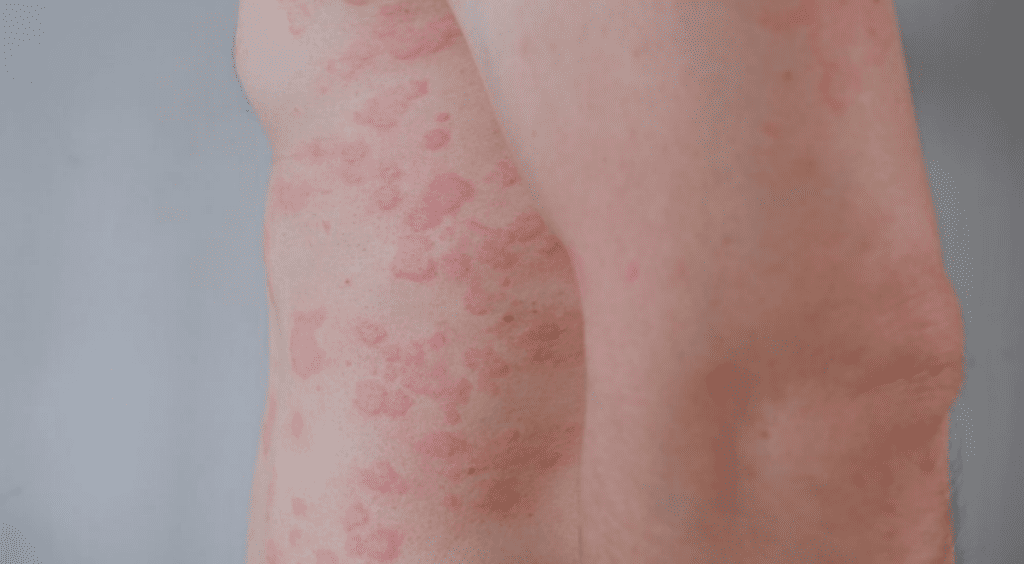
Phase 2 data suggest meaningful skin improvement and an acceptable safety profile
As reported on Healio, litifilimab, an investigational therapy developed by Biogen, demonstrated encouraging efficacy and tolerability in patients with cutaneous lupus erythematosus (CLE), according to new phase 2 findings presented at the 2026 American Academy of Dermatology Annual Meeting in Denver.
Results from part A of the AMETHYST study showed that patients treated with litifilimab experienced faster and greater improvements in skin disease activity compared with those receiving placebo, with differences emerging as early as 4 weeks and sustained through 24 weeks of treatment.
CLE is a chronic autoimmune condition characterized by inflammatory skin lesions that may lead to permanent scarring and disfigurement. Despite its severity, there are currently no FDA‑approved therapies specifically indicated for CLE. In recognition of this unmet need, the FDA granted litifilimab breakthrough therapy designation in January 2026.
Trial design and patient population
The randomized, placebo-controlled phase 2 study enrolled 93 patients with biopsy-confirmed cutaneous lupus and associated systemic manifestations. Participants were assigned to receive either litifilimab plus standard of care (n = 59) or placebo (n = 34), administered every 4 weeks for 24 weeks.
The study population largely reflected the demographics seen in CLE: nearly three-quarters of participants were women, approximately two-thirds were White, and most were receiving concomitant lupus therapies. All patients entered the trial with moderate to severe skin involvement, defined by a Cutaneous Lupus Erythematosus Disease Area and Severity Index Activity (CLASI-A) score of at least 10.
Efficacy outcomes
The primary endpoint was achievement of clear or almost clear skin, measured by a Cutaneous Lupus Activity–IGA–Revised (CLA‑IGA‑R) erythema score of 0 or 1 at week 16. A greater proportion of patients treated with litifilimab met this endpoint compared with placebo, and this separation widened by week 24.
Across multiple secondary endpoints, litifilimab consistently outperformed placebo. Patients receiving the investigational therapy were more likely to experience substantial reductions in CLASI-A scores, including 50% and 70% improvements from baseline. A subset of treated patients also reached minimal or no disease activity by week 24—an outcome not observed in the placebo group.
Investigators highlighted that these clinical improvements reflect both reductions in lesion inflammation and broader improvements across affected skin areas.
Mechanism of action
Litifilimab targets plasmacytoid dendritic cells, inhibiting the production of type I interferons and other proinflammatory mediators believed to play a central role in CLE pathogenesis. According to the study team, suppression of these pathways was observed shortly after the first injection, potentially explaining the rapid onset of clinical benefit.
Safety profile
The treatment was generally well tolerated. Most adverse events reported in the litifilimab group were mild, with nasopharyngitis and headache being the most commonly observed. Although a small number of severe adverse events occurred, no new safety signals were identified over the 24-week treatment period.
Looking ahead
After decades without major therapeutic advances for cutaneous lupus, investigators described the AMETHYST findings as an important step forward. If confirmed in larger and longer-term studies, litifilimab could represent a targeted treatment option for patients with a serious and often disfiguring autoimmune skin disease.
Source: Werth V, et al. Late-breaking research session. Presented at the American Academy of Dermatology Annual Meeting; March 27–31, 2026; Denver.