My story began very suddenly on May 4th, 2025, when I was home from graduate school visiting my family. It had been a great day, shopping and enjoying dinner at my favorite restaurant. I ended the night relaxing on the couch, watching a new Netflix show, when I felt an odd chest pain.
My story began very suddenly on May 4th, 2025, when I was home from graduate school visiting my family. It had been a great day, shopping and enjoying dinner at my favorite restaurant. I ended the night relaxing on the couch, watching a new Netflix show, when I felt an odd chest pain.
I assumed it must be something simple, like a pulled muscle from overdoing it at the gym, and decided to take a hot shower to help ease whatever was going on. After about two minutes in the shower, I could no longer stand. Panicked, I wrapped myself in a towel and crawled to my bedroom. The pain continued to worsen, sharper and deeper, as I managed to scream for help. The paramedics were called and I was loaded into an ambulance. My local hospital performed a scan before labeling me a liability and transferring me to a level-one trauma care center downtown. There, blood work showed extremely elevated liver enzymes, typically around 20 and mine exceeding 1,500, and imaging revealed something I never expected: a giant, hemorrhaged liver tumor.
The term “hepatic adenoma” was foreign to me. I listened as the doctor explained that it was a benign mass of the liver, most often associated with hormonal imbalances. My mind struggled to process what he was saying. I kept thinking, Why did this happen? Could it become cancer? Would it rupture again? I was only 23 years old, too young to even think about my liver failing.
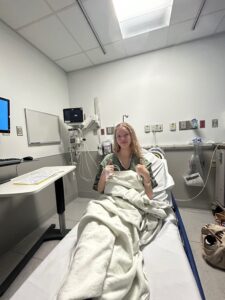 Those first few weeks in the hospital were a whirlwind. I learned that hepatic adenomas are exceedingly rare, about one case per 1,000,000 people overall. Mine had hemorrhaged, causing extensive internal bleeding that put my body into a state of hypovolemic shock and lactic acidosis. The chest pain I thought was a sore muscle was actually a melon-sized tumor pushing against my diaphragm. I was now living with the reality that my liver, something I had never once thought about, could change my entire life.
Those first few weeks in the hospital were a whirlwind. I learned that hepatic adenomas are exceedingly rare, about one case per 1,000,000 people overall. Mine had hemorrhaged, causing extensive internal bleeding that put my body into a state of hypovolemic shock and lactic acidosis. The chest pain I thought was a sore muscle was actually a melon-sized tumor pushing against my diaphragm. I was now living with the reality that my liver, something I had never once thought about, could change my entire life.
Upon meeting with my team of specialists, they explained that hepatic adenomas are typically about 5 cm in size and can be removed via liver resection surgery. Mine, however, was 17 cm and occupying roughly 70% of my liver. It was compressing my stomach, pancreas, hepatic artery, portal vein, and the inferior vena cava of my heart. Because the mass was so large, filled with blood, and touching major blood vessels, removal or transplant were not considered safe options. I waited in the intensive care unit under close monitoring while the doctors worked to determine a path forward. I underwent an arterial embolization procedure to stop the blood supply that was feeding the tumor and prevent further growth. Then, a biliary drain was placed, and I received daily tissue plasminogen activator infusions to break down the clotted blood. My amazing family remained at my bedside through it all, even flying in from out of state to support me.
It was expressed to me by every hepatobiliary surgeon I met that a 17 cm tumor hemorrhaging in the body is typically fatal, with a survival rate of approximately 0.007%. My doctors told me that in all their years of practice, they had never encountered a case like mine. They half-joked that I must have an unusually high pain tolerance, but I can honestly say that initial hemorrhage was the only time I’ve experienced a ten out of ten on the pain scale.
Eventually, I had my drain removed and was finally discharged home on June 24th. Now, the tumor has shrunk by roughly 40% and continues to diminish every day.
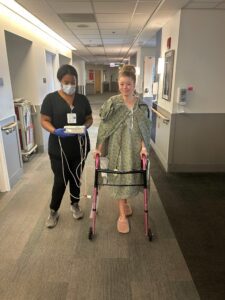 But physical recovery is only part of the story, because there’s a particular kind of mourning that accompanies serious illness. I wrestled with guilt, wondering if I should have recognized something sooner, even though there were no warning signs. I questioned my own intuition, asking how I didn’t sense something was wrong. How long had an eight-pound tumor been growing inside my body without my knowledge? I had to learn to forgive the version of myself that existed before all of this happened.
But physical recovery is only part of the story, because there’s a particular kind of mourning that accompanies serious illness. I wrestled with guilt, wondering if I should have recognized something sooner, even though there were no warning signs. I questioned my own intuition, asking how I didn’t sense something was wrong. How long had an eight-pound tumor been growing inside my body without my knowledge? I had to learn to forgive the version of myself that existed before all of this happened.
Illness has reshaped my relationships as well. Losing friends who don’t understand that “bad days” can be completely debilitating, even when I might appear healthy. Not to mention, the world outside the hospital kept moving. My classmates continued their program and reached milestones I had planned to share with them. I will not graduate alongside the cohort I began with, and accepting that reality required its own healing.
There’s so much more that goes unmentioned: the endless CTs, MRIs, EKGs, echocardiograms, X-rays, blood tests, Holter monitors, and of course the dozens of nurses, doctors, residents, Panera Agave Lemonade orders following 30+ hour NPO fasts, Zoom classes from my hospital bed, and gift baskets that helped me survive such a challenging and unpredictable time. More recently, I’ve learned to adjust rather than wallow. I prioritize follow-up appointments with specialists, listening to my body, and shifting my mindset toward gratitude for the fact that I survived something so severe. I carry a deep appreciation for the incredible physicians who saved my life, and I’m also so fortunate to connect with other patients who understand the language and hardships of liver disease.
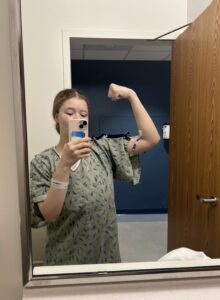 Returning to school feels significant in a full-circle kind of way, mostly because my new clinical placement is in the very ICU that I was hospitalized in just months ago. I know this experience has shaped me as a future healthcare provider, as my empathy for patients has only deepened by understanding firsthand what it feels like to be on the other side of care.
Returning to school feels significant in a full-circle kind of way, mostly because my new clinical placement is in the very ICU that I was hospitalized in just months ago. I know this experience has shaped me as a future healthcare provider, as my empathy for patients has only deepened by understanding firsthand what it feels like to be on the other side of care.
My life may not look the way it once did, but it’s still mine. And that’s what keeps me going every day. If I could say one thing to someone newly diagnosed with HCA, it would be this: There’s a long road of recovery ahead, but you’re definitely not alone in this fight.