I’ve learned something brutal over the last few weeks:
Most people cannot tolerate the reality of a child nearly dying. So they dilute it. They soften it. They reach for platitudes so they don’t have to sit with the truth.
This post is not for comfort.
It’s for accuracy.
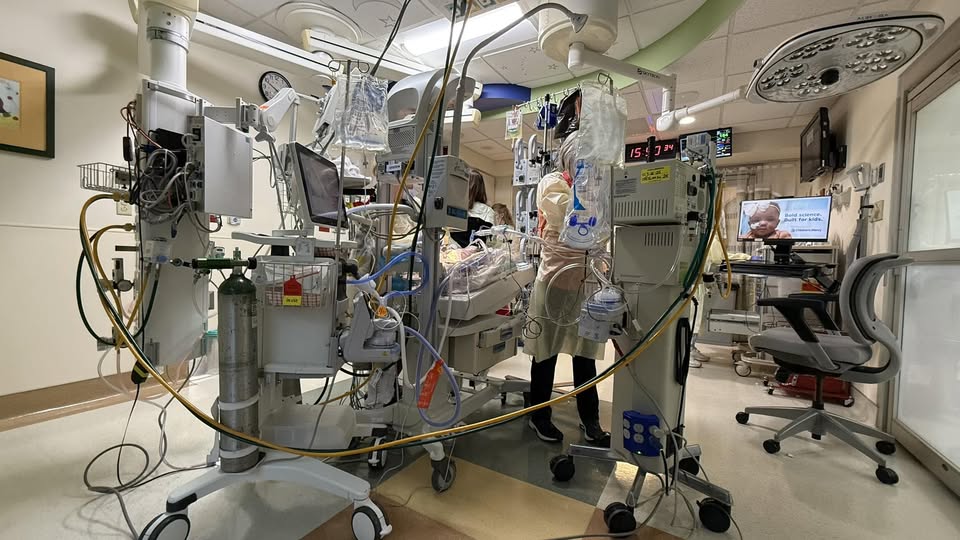
Our daughter has spent weeks in the ICU fighting for her life. Not in an inspirational, hashtag-worthy way. In a sustained, clinically documented, “we might lose her tonight” way – repeatedly.
She has cystic fibrosis and was born with a severe bowel obstruction. Since birth, surgeons have cut into her body again and again, removing sections of intestine because they were dead. Not at risk. Not compromised. Dead tissue inside a newborn.
At one point, her abdomen was left open because closing it would have killed her. Her organs were too swollen, too unstable, too close to catastrophic failure to be put back inside her body. We stood there knowing her insides were exposed, knowing infection, pressure, or one wrong physiologic shift could end her life.
That alone should have been enough fear for a lifetime.
It wasn’t.
She began bleeding internally. Her body entered a state where it could not decide whether to clot or hemorrhage, so it did both. She bled into her lungs. She stopped being able to breathe. The machines meant to keep her alive stopped being enough.
Standard life support failed.
She was escalated to one of the most extreme forms of ventilation available, the kind used when doctors are no longer confident survival is the most likely outcome. She had to be sedated and paralyzed – not for comfort, but because her body could not tolerate being awake and alive at the same time.
Here is the part people never want spelled out:
We were afraid all the time.
Not anxious. Not worried. Afraid.
Afraid to leave the room.
Afraid to sleep.
Afraid when an alarm changed pitch.
Afraid when footsteps approached too quickly.
Afraid when the room got quiet.
We watched her blood pressure collapse. We watched her platelet count fall to levels where spontaneous bleeding becomes a real possibility. We were told about blood clots. We watched parts of her body lose circulation. Doctors discussed permanent damage to her hand because blood flow was failing.
There were moments when the room felt heavy and controlled and deliberate – and we knew exactly why.
Doctors don’t slow down and choose their words carefully when things are fine.
They do that when they don’t know how the story ends.
There were nights when we mentally rehearsed what life would look like if she didn’t survive. Not because we wanted to. Because when the risk is real, your brain prepares whether you give it permission or not.
Hope felt reckless.
Fear felt rational.
So when someone says, “At least she’s stable now,” understand what that actually means in an ICU:
It means death is not actively occurring at this exact second.
When someone says, “Kids are resilient,” what they’re really doing is creating emotional distance between themselves and the reality that a baby almost died.
When someone says, “She looks better,” they are seeing skin – not the machines, medications, paralysis, anticoagulation, vigilance, and constant intervention keeping her alive.
She didn’t bounce back.
She didn’t fight through.
She endured – so far – because modern medicine is holding the line minute by minute.
Even now, she is not safe. She is not “out of the woods.” She is alive because her body is being continuously managed, corrected, supported, and watched. Every improvement comes paired with the knowledge that one infection, one bleed, one failure could send us straight back to the edge.
This experience didn’t scare us.
It reprogrammed us.
It taught us what real fear feels like – the kind that embeds itself in your nervous system, hijacks your sleep, and follows you even when you leave the hospital. The kind that doesn’t disappear when numbers improve or machines get quieter.
So if we seem distant, sharp, hollow, guarded, or fundamentally altered – this is why.
And if this post makes you uncomfortable, understand this clearly:
Your discomfort is the cost of hearing the truth.
Living it costs infinitely more.
We are grateful she is still here.
But this has been the most terrifying, life-altering experience of our lives.
And we are still in it.
If you cannot sit with how close this came to ending differently – if you need to minimize it to protect yourself – do not offer reassurance. Do not soften it. Do not reframe it. Silence is the only response that doesn’t do harm.
Update from Mom:
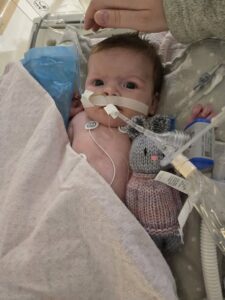 Delilah is improving every day! We’re not 100% out of the woods yet but everything is trending in the right direction finally. All of her brain scans have been totally normal. She is almost off the ventilator. They have started feeding her to wake up her guts. Her stoma is working properly. She is going to lose a couple of fingertips because when her body was fighting extremely hard to keep her organs alive it deemed fingers less important at that time, witch is fair. Incredible battle scars for such a little fighter.
Delilah is improving every day! We’re not 100% out of the woods yet but everything is trending in the right direction finally. All of her brain scans have been totally normal. She is almost off the ventilator. They have started feeding her to wake up her guts. Her stoma is working properly. She is going to lose a couple of fingertips because when her body was fighting extremely hard to keep her organs alive it deemed fingers less important at that time, witch is fair. Incredible battle scars for such a little fighter.