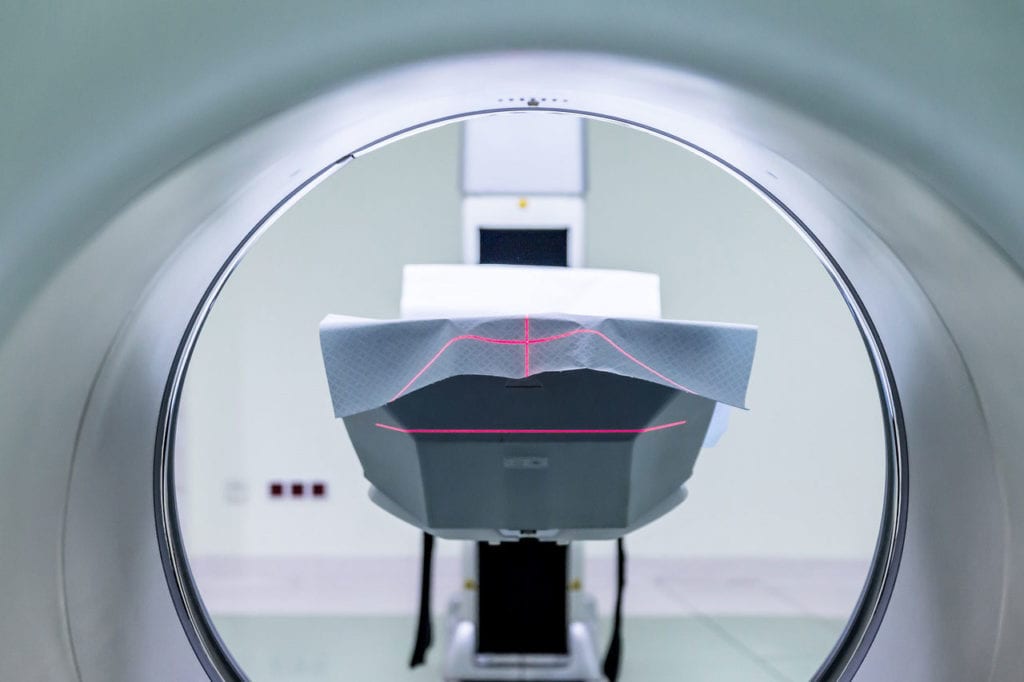
To monitor this risk, Resnick goes through the standard recommended protocol for individuals with a risk of at least 20%. This includes mammograms, ultrasounds, and MRIs which alternate every 6 months. The MRI using gadolinium contrast is the most sensitive of all of these tests, and therefore it truly is best to use all three in conjunction with one another. After the first MRI, a baseline is established that can then be quickly compared year to year.
Resnick herself has had 6 different MRIs over the last 8 years. As a whole, it’s a good monitoring system. But there is a problem. Some of the gadolinium (which is an earth metal) is retained in some patients following the test.
Unfortunately, doctors still don’t understand everything about how gadolinium retention in the body can affect people long-term. In other words, they just don’t know how safe MRIs truly are.
“What’s worse — a known risk for breast cancer or an undetermined risk for the diagnostic tool used to detect it?”
Think X-rays.
X-Rays
At age 38, Resnick’s sister was diagnosed with breast cancer and faced surgery and reconstruction. That was now 4 decades ago.
What’s different between Resnick and her sister, is that her sister had none of the same risk factors that Resnick does besides her heritage. There wasn’t even a documented family history at the time she was diagnosed, as she was the first one in the family to receive this kind of news.
It turns out that her sister had an unknown risk. She had undergone a series of x-rays during puberty in effort to diagnose, and then treat, her scoliosis. Back then the risk of developing cancer due to x-ray exposure was not known. Now, we clearly understand the risk of this radiation. There is a strong correlation between young women who are given x-rays to monitor scoliosis and breast cancer. It is even now a standard question asked on mammogram intake forms.
What if the use of MRIs is soon correlated with the same type of risk?
Risks with MRIs?
The problem is that we don’t know what we don’t know until we know it. The FDA began analyzing the effects of long term gadolinium retention back in 2017. Gadolinium can be retained in various parts of the body, including the brain, for years following a routine MRI.
The FDA concluded at that time that the benefits of the screening still outweighed the potential risk. However, they also attached a new warning to MRIs stating that patients must be given a guide discussing potential risk before the MRI is given.
That’s not exactly reassuring.
They also stated that some factors may put individuals at an increased risk for retaining gadolinium. This includes people who are pregnant, have an inflammatory condition, require lifetime doses of gadolinium, and children. It was previously understood that those with poor kidney function had heightened risk of retention, but now, although researchers still aren’t sure what this retention means, they at least have a better understanding of who else might be at risk. Doctors are now encouraged to evaluate these retention characteristics when they are deciding on a treatment agent.
In the long term, what could this retention cause? Dementia, sensory loss, heightened anxiety, or brain cancer? Are the unknown risks likely enough that individuals should minimize their MRIs? What if these MRIs are used as part of their routine cancer screening due to their known, heightened risk of cancer?
“This much I know: The MRI with contrast helps my doctors navigate this blizzard inside me.” – Meredith Resnick
Resnick’s 7th MRI is coming soon. She’s trying to not think about all of the “what ifs” and focus on what she needs in the present. But its scary to know that even the most brilliant researchers still do not know everything in the medical field. We are still learning and growing, and unfortunately, taking risks, together.
You can read more about Resnick’s personal story here.