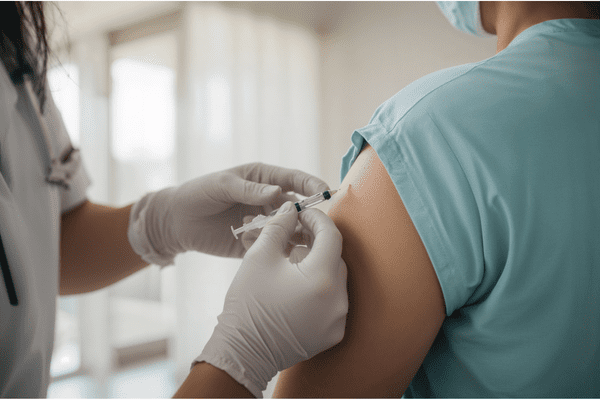
As reported on Science Daily, a breast cancer vaccine tested more than 20 years ago is drawing renewed scientific interest after researchers discovered that every participant in the original trial remains alive—an extraordinary outcome for individuals who once had metastatic disease. A new analysis suggests that the vaccine may have triggered unusually durable immune memory, offering insights that could reshape future cancer‑immunotherapy strategies.
Unexpected Longevity From an Early Vaccine Trial
The original trial, conducted at Duke Health and led by immunologist Herbert Kim Lyerly, M.D., enrolled women with advanced breast cancer. Survival lasting decades is exceedingly rare for metastatic cases, prompting investigators to revisit the participants’ immune profiles. What they found was striking: the women continued to harbor immune cells capable of recognizing cancer long after the initial vaccination.
These cells were marked by the molecule CD27, a signal involved in maintaining long-term immune memory. The findings, published in Science Immunology, suggest that amplifying CD27 activity could significantly bolster vaccine performance.
Enhancing Tumor Elimination Through CD27 Activation
To test this idea, researchers turned to mouse models. They combined a vaccine targeting the HER2 protein—a common driver in certain breast cancers—with an antibody engineered to stimulate CD27. The combination therapy produced far better outcomes than the vaccine alone: roughly 40% of treated mice cleared their tumors, compared with just 6% receiving only the vaccine.
Further investigation revealed that this enhancement stemmed largely from CD4+ T cells, a cell type often overshadowed in cancer research by cytotoxic CD8+ T cells.
An Underappreciated Immune Player Takes Center Stage
Traditionally regarded as “helper” cells, CD4+ T cells are now emerging as potential central drivers of long-term anti‑tumor immunity. In the Duke experiments, boosting CD27 dramatically strengthened their ability to coordinate a wide-ranging immune response. When the researchers also supported CD8+ T cells with a second antibody, tumor rejection rates surged to nearly 90% in mice.
The results indicate that designing cancer vaccines around the capabilities of CD4+ T cells—rather than focusing solely on tumor‑killing CD8+ cells—may be essential to achieving durable clinical benefit.
Potential Pathway to More Effective Cancer Vaccines
One promising aspect of the approach is its simplicity: the CD27‑boosting antibody only needed to be administered once, at the same time as the vaccine. This single‑dose synergy may make it easier to integrate the strategy with widely used treatments such as checkpoint inhibitors and antibody–drug conjugates.
Researchers believe these insights could finally unlock the potential that cancer vaccines have long shown but rarely delivered in practice.